Explore Our Vein Treatments
At Vein Treatment Clinic, we only focus on the latest vein procedures that cause minimal pain or discomfort, either during or after treatment.
Select the vein condition you want to explore
Spider veins
Varicose veins
Chronic venous
insufficiency
Spider Veins
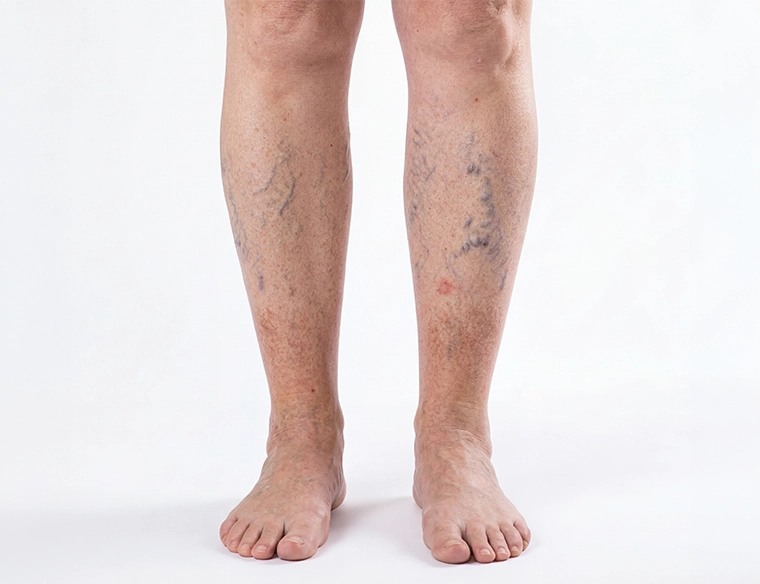
Causes
Spider veins develop when small superficial blood vessels become dilated due to increased pressure inside the veins or weakness in the vein walls. They are often associated with underlying venous insufficiency but can also occur independently.
When tiny vein valves do not function efficiently, blood can pool in superficial vessels, causing them to enlarge and become visible through the skin. Hormonal changes and genetic predisposition can also contribute to their development.
Risk factors include but are not limited to:
- Family history of spider veins or varicose veins
- Hormonal changes, including pregnancy, menopause, or use of hormonal therapy
- Prolonged standing or sitting
- Aging and natural weakening of vein walls
- Obesity or increased abdominal pressure
- Previous vein disease or venous insufficiency
- Sun exposure
- History of blood clots or vein inflammation
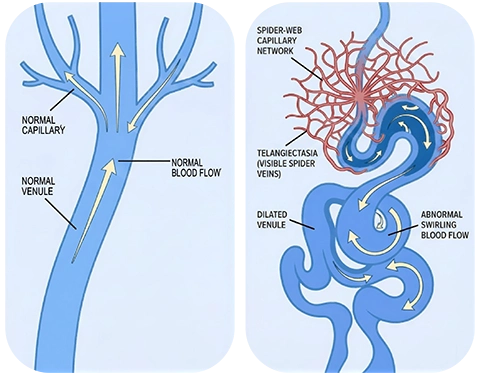
Symptoms
Spider veins are often considered a cosmetic concern, but they may also be associated with mild symptoms, including:
- Thin red, blue, or purple veins visible near the surface of the skin
- Web-like or branching vein patterns
- Mild burning or itching in the affected area
- Leg heaviness or fatigue
- Mild swelling, especially after prolonged standing
- Tenderness around clusters of veins
In some cases, spider veins may indicate underlying venous insufficiency, which is why a vein evaluation can help determine whether additional treatment is recommended.
Varicose Veins
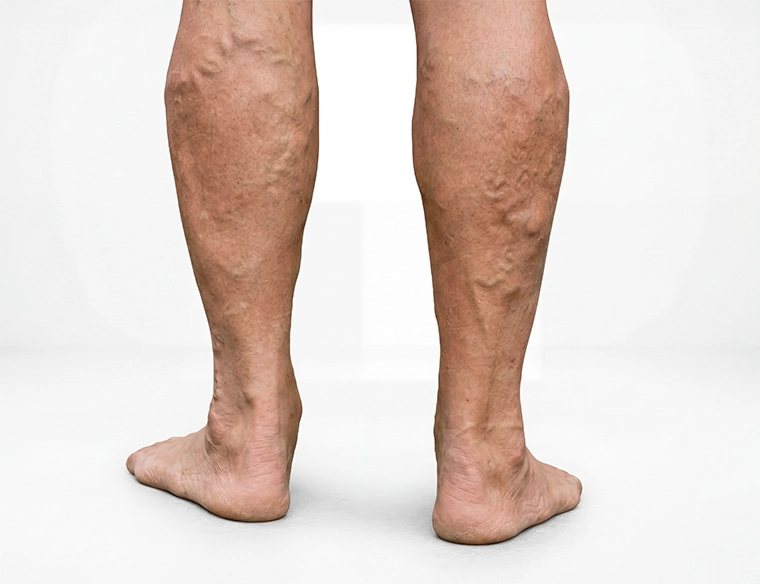
Causes
Varicose veins develop due to chronic venous insufficiency, a condition in which the one-way valves inside leg veins weaken or fail. When these valves do not close properly, blood flows backward and pools in the vein instead of returning efficiently to the heart.
This increased pressure causes veins to enlarge, stretch, and become twisted or bulging over time. As pressure builds, vein walls weaken, which can lead to visible varicose veins and progressive vein disease if left untreated.
Risk factors include but are not limited to:
- Family history of varicose veins or venous insufficiency
- Prolonged standing or sitting
- Pregnancy and hormonal changes
- Aging
- Obesity or increased abdominal pressure
- History of blood clots
- Prior vein inflammation
- Lack of regular physical activity
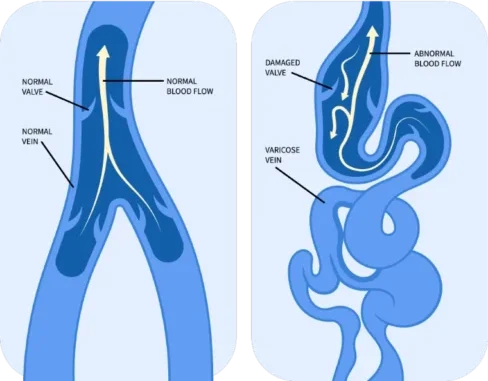
Symptoms
Varicose veins may be visible and symptomatic, though some patients experience mild or no discomfort at first. Common symptoms include:
- Large, twisted, bulging veins in the legs
- Leg heaviness or fatigue, especially at the end of the day
- Aching, throbbing, or burning sensations
- Swelling in the ankles or lower legs
- Nighttime leg cramps
- Itching around affected veins
- Skin discoloration near the ankles
- Hardening of the skin or tissue
In more advanced cases, untreated venous insufficiency can lead to skin changes or venous ulcers. A vein ultrasound evaluation helps determine the severity of reflux and guide appropriate treatment.
Chronic Venous Insufficiency
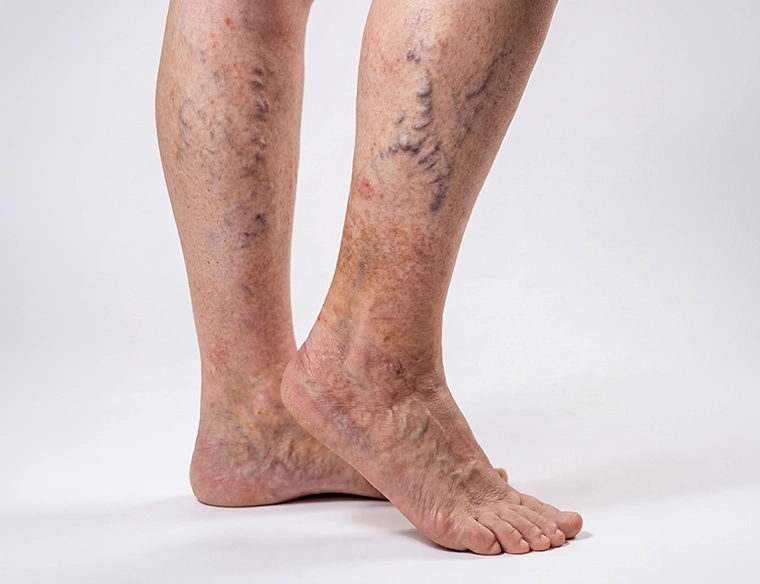
Causes
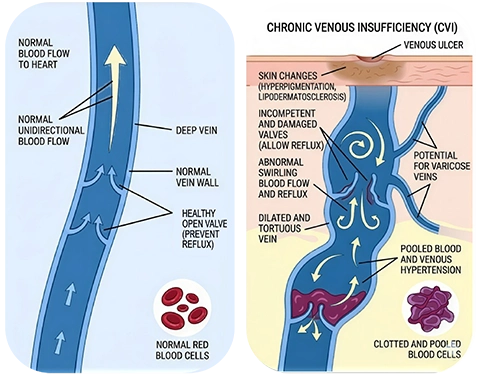
Chronic Venous Insufficiency (CVI) occurs when the valves inside the leg veins do not function properly, allowing blood to flow backward (venous reflux) and pool in the lower extremities instead of returning efficiently to the heart.
Over time, this persistent pressure damages vein walls, stretches the veins, and impairs circulation. CVI is a progressive condition and is the underlying cause of many cases of varicose veins and advanced vein disease.
Risk factors include but are not limited to:
- Family history of venous insufficiency or varicose veins
- Prior deep vein thrombosis (DVT)
- Prolonged standing or sitting
- Pregnancy and hormonal changes
- Age over 50
- Obesity
- Sedentary lifestyle
- Previous leg injury or vein inflammation
Symptoms
Chronic venous insufficiency symptoms often worsen over time and may affect daily comfort and mobility. Common signs include:
- Persistent leg heaviness or fatigue
- Aching, throbbing, or burning pain in the legs
- Swelling in the ankles and lower legs
- Visible varicose veins
- Skin discoloration around the ankles
- Dry, itchy, or inflamed skin
- Hardening or thickening of the skin
- Slow-healing wounds or venous leg ulcers in advanced cases
Because CVI is a progressive condition, early evaluation with a venous ultrasound can help identify reflux and guide appropriate treatment before complications develop.
No matter your condition, our doctors
can help you experience relief today!
- Minimally invasive
- Cutting edge
- Zero downtime
Vein Treatments
Select the treatment you want to check
Sclerotherapy
Radiofrequency
Ablation (RFA)
Endovenous Laser
Treatment (EVLT)
Compression
therapy
Phlebectomy
Sclerotherapy
Sclerotherapy is a minimally invasive vein treatment where a doctor injects a special medication, called a sclerosant, directly into an unhealthy vein. This medication irritates the vein walls, making the vein collapse, seal shut, and gradually fade from view.
Procedure time
30-60 min
Recovery
Fast
Downtime
Zero
Likelihood of Insurance Coverage
HIGH
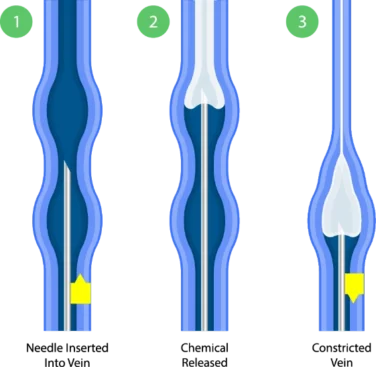
How Does Sclerotherapy Works?
Sclerotherapy is a minimally invasive procedure where a medication is injected into an unhealthy vein. The medication irritates the vein walls, causing the vein to collapse and close off. Blood naturally reroutes to healthier veins, and the body gradually absorbs the treated vein.
Who Can Receive Sclerotherapy?
This procedure is a safe and effective treatment option for most patients experiencing symptoms from spider veins. The procedure requires a comprehensive consultation and an ultrasound mapping of your veins to determine if you are a suitable candidate.
Pros and Cons of Sclerotherapy
- Minimally invasive, non-surgical treatment: Sclerotherapy treats spider veins and small varicose veins through a simple in-office injection.
- Highly effective for spider veins: It significantly reduces or eliminates visible spider veins in most patients.
- No anesthesia and minimal downtime: The procedure is performed in a vein clinic setting, and patients usually return to normal activities the same day.
- Quick treatment sessions: Most appointments last 15–30 minutes.
- Improves appearance and mild symptoms: It can reduce visible veins as well as mild discomfort such as burning or itching.
- Proven and widely used treatment: Sclerotherapy has been safely performed for decades and remains a standard treatment for spider veins.
- Best for spider veins and small veins: Larger varicose veins caused by deeper venous reflux may require additional treatments.
- Multiple sessions may be needed: Some patients require more than one session for optimal results.
- Results develop gradually: Treated veins fade over several weeks as the body absorbs them.
- Temporary side effects are possible: Mild bruising, swelling, or temporary discoloration may occur but typically resolve on their own.
How to Find a Sclerotherapy Specialist?
Choosing a specialist with extensive experience in Sclerotherapy is key to achieving the best cosmetic and medical results. Our vein specialists are highly skilled in this procedure, ensuring optimal outcomes.
Radiofrequency Ablation (RFA)
Radiofrequency Ablation (RFA), also known as VNUS or ClosureFAST, is a Medicare-approved, minimally invasive technique for eliminating unhealthy veins. RFA uses thermal (heat-based) energy to damage the vein, causing it to seal closed. RFA is used to treat major varicose veins and is a safer and more effective alternative to surgery.
Procedure time
Recovery
Fast
Downtime
Zero
Likelihood of Insurance Coverage
HIGH
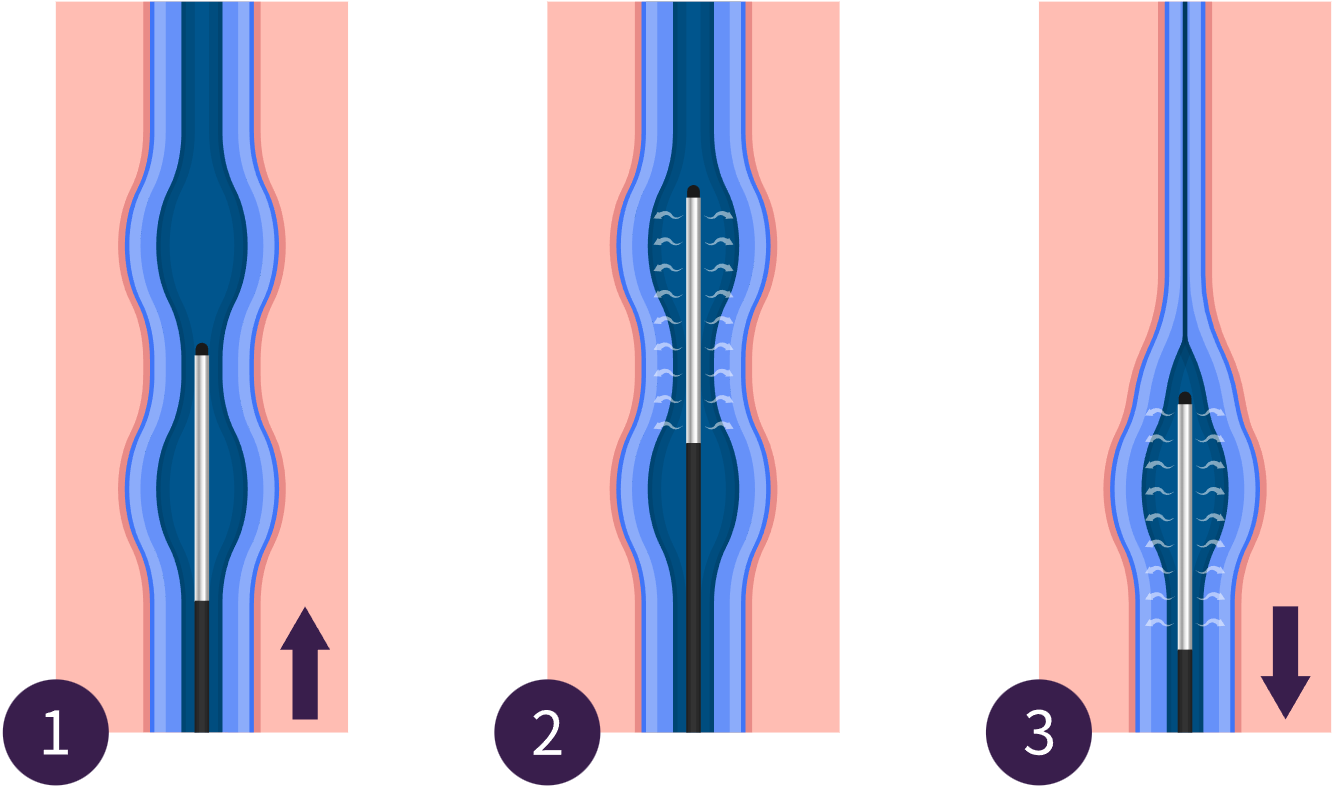
How Does Radiofrequency Ablation Works?
Radiofrequency Ablation (RFA) seals the underlying diseased vein, which is often the source of varicose veins. The procedure involves inserting a thin catheter under ultrasound guidance. This catheter then delivers controlled radiofrequency energy to the vein walls, heating them to close off the problematic vein.
Who Can Receive Radiofrequency Ablation?
Candidates are typically people with varicose veins caused by underlying venous insufficiency. We confirm this condition with an ultrasound evaluation. RFA effectively treats the source of the problem. This allows your body to redirect blood flow into healthier veins.
Pros and Cons of Radiofrequency Ablation
- Minimally invasive treatment for venous insufficiency: Radiofrequency ablation (RFA) treats the underlying cause of varicose veins by closing diseased veins using controlled heat energy.
- Highly effective for larger varicose veins: RFA is commonly used to treat great saphenous and small saphenous vein reflux, with strong long-term success rates.
- Performed in-office under local anesthesia: The procedure is done in a vein clinic setting without general anesthesia.
- Minimal downtime and fast recovery: Most patients walk immediately after treatment and return to normal activities within 24 hours.
- Relieves symptoms as well as appearance: RFA can improve leg pain, heaviness, swelling, fatigue, and other symptoms caused by venous insufficiency.
- Reduces the risk of disease progression: By treating reflux at the source, RFA helps prevent worsening varicose veins and related complications.
- Not typically used for very small spider veins: RFA treats larger refluxing veins; smaller surface veins may still require treatments like sclerotherapy.
- Mild post-procedure discomfort may occur: Temporary tightness, bruising, or soreness along the treated vein is possible but usually resolves quickly.
- Compression stockings are usually recommended: Patients are often advised to wear compression stockings for a short period after treatment.
- Requires ultrasound-guided evaluation: A venous ultrasound is necessary to confirm reflux and determine candidacy.
- Does not prevent new vein disease from developing: While treated veins remain closed, new reflux can develop over time in predisposed patients.
How to find a Radiofrequency Ablation Specialist?
Choosing a specialist with extensive experience in Radiofrequency Ablation is key to achieving the best cosmetic and medical results. Our vein specialists are highly skilled in this procedure, ensuring optimal outcomes.
Endovenous Laser Treatment (EVLT)
Endovenous Laser Treatment (EVLT) addresses the underlying vein disease rather than just the visible symptoms. This treatment is widely used as a first-line therapy for diseased superficial veins and is supported by extensive clinical evidence demonstrating its safety, effectiveness, and long-term results.
Procedure time
Recovery
Fast
Downtime
Zero
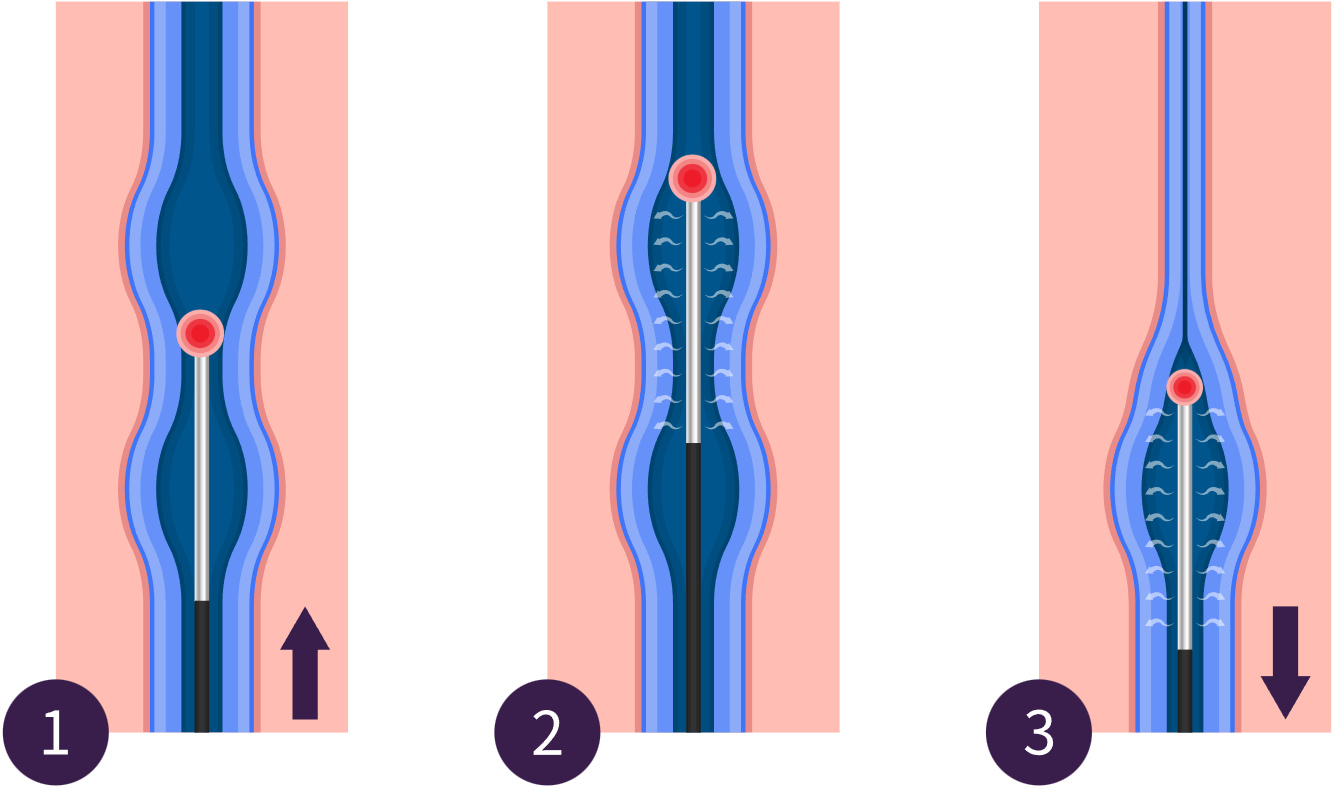
How Does Endovenous Laser Treatment Works?
Endovenous Laser Treatment (EVLT) is a heat-based, minimally invasive laser treatment for varicose veins. Like RFA, it uses ultrasound mapping to guide a thin fiber. We insert this fiber into the diseased vein. The fiber delivers laser energy. This laser energy heats the vein walls, permanently closing the vein. People sometimes refer to this procedure as EVLA vein treatment.
Who Can Receive Endovenous Laser Treatment?
This procedure is for patients with a significant need for varicose vein treatment due to underlying venous reflux. It’s determined by a comprehensive consultation, which includes ultrasound mapping.
How to Find a Endovenous Laser Treatment Specialist?
Choosing a specialist with extensive experience in Endovenous Laser Treatment is key to achieving the best cosmetic and medical results. Our vein specialists are highly skilled in this procedure, ensuring optimal outcomes.
Compression Therapy
Compression therapy is a non-invasive medical treatment that uses controlled pressure applied to the limbs to support circulatory and lymphatic health. It is widely used in both preventive and post-operativecare, particularly for conditions affecting the veins.
Procedure time
Improve
Symptoms
Zero
Downtime
Essential for Post-op Recovery
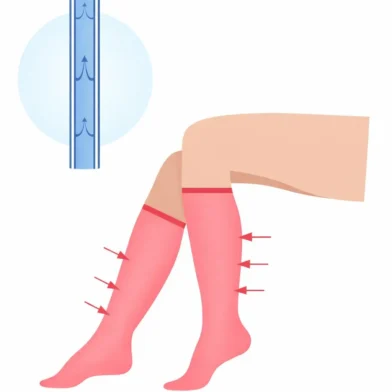
How Does Compression Therapy Works?
Compression therapy uses specially designed elastic stockings to apply graduated pressure to the legs. The pressure is strongest at the ankle and decreases as it moves up the leg, improving venous return, reducing pooling and swelling, and relieving symptoms.
Who Can Receive Compression Therapy?
This therapy is a versatile support option for anyone with venous insufficiency, spider veins, or varicose veins. It serves as a conservative first step to support leg health and is a key part of post-procedure recovery. A specialist will determine the specific pressure level (mmHg) required to provide optimal support based on your symptoms.
How to Find a Vein Specialist?
Choosing a specialist with extensive experience in venous diseases is key to achieving the best cosmetic and medical therapy. Our vein specialists are highly skilled in diagnosis and treatments, ensuring optimal health for the patients.
Phlebectomy
Ambulatory phlebectomy is a treatment used to remove superficial varicose veins, typically in the legs. It is performed as an outpatient procedure, meaning the patient can return home the same day, and it does not require general anesthesia.
Procedure time
Recovery
Downtime
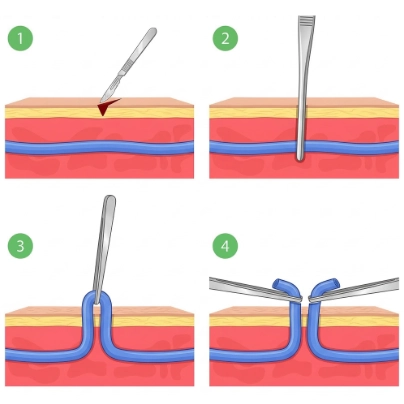
How Does Ambulatory Phlebectomy Works?
Ambulatory phlebectomy is a minimally invasive procedure where a doctor removes bulging varicose veins through tiny skin incisions. After numbing the area with local anesthesia, specialized micro-hooks are used to extract diseased vein segments. The incisions are so small that they typically require only adhesive strips rather than traditional stitches, and blood naturally reroutes to deeper, healthier veins.
Who Can Receive Ambulatory Phlebectomy?
This treatment is ideal for patients with superficial varicose veins causing pain, swelling, or cosmetic concerns. A consultation and ultrasound mapping are required to confirm candidacy and check for underlying venous insufficiency.
How to Find a Ambulatory Phlebectomy Specialist?
Choosing a specialist with extensive experience in Ambulatory Phlebectomy is key to achieving the best cosmetic and medical results. Our vein specialists are highly skilled in this procedure, ensuring optimal outcomes.
Let our doctors customize your treatment plan
Finding relief is as simple as filling this quick form below:
Thank you, your request has been submitted
One of our team members will reach out to you shortly
If you'd prefer immediate assistance, call us directly: (844) 297-2300



